Orthopedic surgeries carry a higher risk of blood clot formation, which can become a serious health concern if not addressed promptly. This guide focuses on practical prevention strategies to help reduce clotting risk, support recovery, and minimize complications, allowing patients to heal more safely and with greater confidence.
Understanding Blood Clots
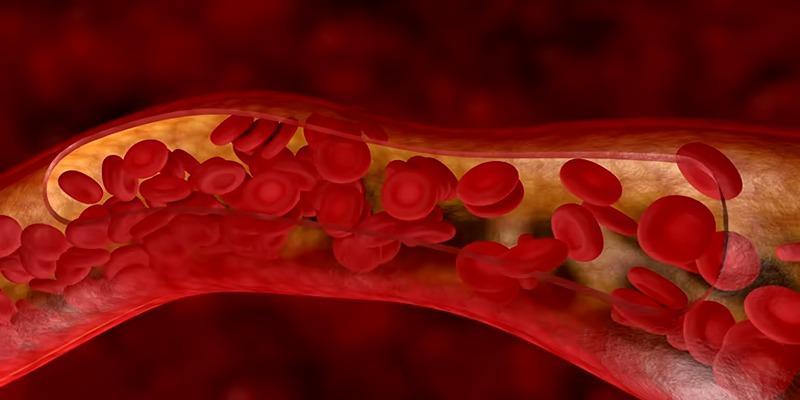
Deep vein thrombosis (DVT) occurs when blood thickens and forms a clot, most commonly in the legs. These clots can restrict normal blood flow, leading to swelling and pain. In more severe cases, a clot may travel to the lungs and cause a pulmonary embolism, which can be life-threatening. For patients recovering from orthopedic surgery, understanding how and why blood clots form is especially important, as several risk factors often overlap during this period.
Causes of Blood Clots After Orthopedic Procedures
After orthopedic surgery, multiple factors may contribute to an increased risk of clot formation. Identifying these causes allows patients and healthcare providers to take targeted preventive steps and reduce the likelihood of complications.
Immobility
Reduced movement during the postoperative period is one of the most significant contributors to blood clots. Patients are often required to rest or limit activity after surgery, which can slow blood flow in the legs. When circulation decreases, conditions become more favorable for clot development. Even light movement, when approved by a healthcare provider, or the use of compression methods can help counteract this risk.
Tissue Damage
Orthopedic procedures frequently involve manipulation of bones and surrounding soft tissues, which can temporarily damage blood vessels. This triggers the body’s natural clotting response as part of healing. While this response is normal, excessive clot formation can lead to dangerous blockages. For this reason, surgical techniques aim to minimize tissue trauma whenever possible.
Pre-existing Medical Conditions
Certain underlying conditions can further increase the likelihood of postoperative blood clots. Factors such as obesity, smoking, or a personal history of clotting disorders are commonly involved. Patients with these risks often require closer monitoring and individualized prevention plans, which may include anticoagulant medication or specific lifestyle adjustments.
Preventative Measures
Preventing blood clots after orthopedic surgery usually requires a combination of approaches rather than relying on a single method. Medications, physical activity, and supportive devices often work together to improve circulation and support recovery.
Anticoagulant medications, commonly known as blood thinners, are frequently prescribed to lower the risk of clot formation. These medicines reduce the blood’s tendency to clot while being carefully monitored to avoid excessive bleeding. For this reason, following dosage instructions and attending follow-up appointments play an important role in maintaining both safety and effectiveness during recovery.
In addition to medication, compression stockings or mechanical compression devices are often recommended to promote healthy blood flow. By applying gentle, consistent pressure to the lower limbs, these devices help reduce venous pooling and are particularly helpful for patients with limited mobility after surgery. When used as directed, they can provide steady circulatory support throughout the recovery period.
Movement is another key factor in clot prevention. When medically appropriate, early mobility and guided physical therapy help keep blood flowing and reduce the chance of pooling in the legs. Even simple activities, such as ankle exercises in bed or short, supervised walks, can contribute meaningfully to circulation. Alongside movement, proper hydration helps prevent blood from becoming overly thick, while a balanced diet supports overall vascular health. Nutrients such as omega-3 fatty acids, fiber, and antioxidants may help reduce inflammation and complement other preventive measures.
Recognizing Symptoms
Being able to recognize the warning signs of blood clots allows for faster medical intervention, which is especially important during the postoperative recovery period. Symptoms can vary depending on where a clot forms, so awareness of common indicators is essential.
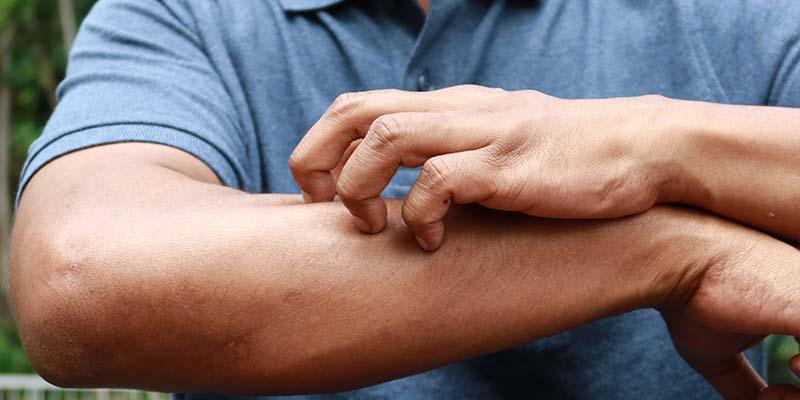
Swelling in one arm or leg, particularly when accompanied by pain or tenderness, may suggest the presence of a clot. The affected area can feel warm or appear noticeably swollen due to restricted blood flow and should be evaluated promptly. Changes in skin color can also occur, with the skin near a clot appearing red, discolored, or warm to the touch. These visible changes often serve as early warning signs and should not be overlooked.
In more serious cases, symptoms may affect breathing. Sudden or unexplained shortness of breath can indicate a pulmonary embolism, a condition that requires immediate medical attention. This may occur alongside chest pain, a rapid heartbeat, or feelings of light-headedness, all of which signal the need for urgent care.
Treatment Options
When blood clots are identified early, treatment outcomes are generally more favorable. Treatment plans vary based on clot location and severity.
Anticoagulant Medication
Anticoagulants are commonly used to prevent existing clots from growing and to reduce the risk of new clots forming. Medications such as heparin or warfarin work by interfering with the clotting process and often require regular monitoring.
Thrombolytic Therapy
In severe or life-threatening cases, thrombolytic medicines may be used to dissolve clots quickly. These medications are administered under close medical supervision due to bleeding risks and are typically reserved for emergency situations.
Compression Therapy
Compression therapy can also support treatment by improving venous blood flow and reducing swelling. When combined with medication, it may help prevent long-term complications such as post-thrombotic syndrome.
Patient Education
Patient awareness plays a key role in preventing complications. Staying active as advised, following prescribed treatments, and recognizing early warning signs all contribute to better recovery outcomes. Ongoing education helps patients take an active role in their own care.

Conclusion
Reducing blood clot risk after orthopedic surgery depends on consistent preventive care and early awareness. By following medical guidance, maintaining appropriate movement, and responding quickly to symptoms, patients can significantly improve recovery outcomes. Proactive management and informed decision-making help ensure a safer and more successful healing process.